Obstetric Anal Sphincter Injuries (OASIS)
An OASIS injury can have a devastating effect on the life of a young mother who develops incontinence of flatus and faeces.
This can happen because the sphincter transections are either not identified ; not repaired correctly or the repair subsequently breaks down. Over time ,especially during the menopause even good repairs can weaken because of progressive loss of smooth muscle and connective tissue.
The External Anal Sphincter (EAS) is comprised of striated muscle and is innervated by the pudendal nerve. The Internal Anal Sphincter (IAS) is comprised of smooth muscle and is innervated by the autonomic nerves. The IAS is responsible for 70-80% of fecal continence and remains in a permanent state of contraction to achieve this.
If a true mediolateral episiotomy is inserted the risk to the sphincters is substantially reduced for forceps deliveries and to a lesser extent vacuum extractions and in primipara is certainly warranted .It can reduce the risk of an OASIS injury from forceps by 10-fold.
The repair of sphincters commences with identification of the injury. This is best achieved by a careful rectal examination at the time of episiotomy repair. With the standard use of rectal doses of NSAID’s for analgesia after delivery there is a golden opportunity to detect an OASIS injury. An injury to the IAS should be repaired separately from any EAS injury. The IAS is more deceptive than the IAS as it resembles fascia rather than muscle and it lies cephalad of the EAS. The postoperative care of an OASIS injury should include prophylactic antibiotics, prescription of aperients and referral for pelvic floor physiotherapy.
There is probably a case for referral to a colorectal surgeon in many cases of OASIS injury.
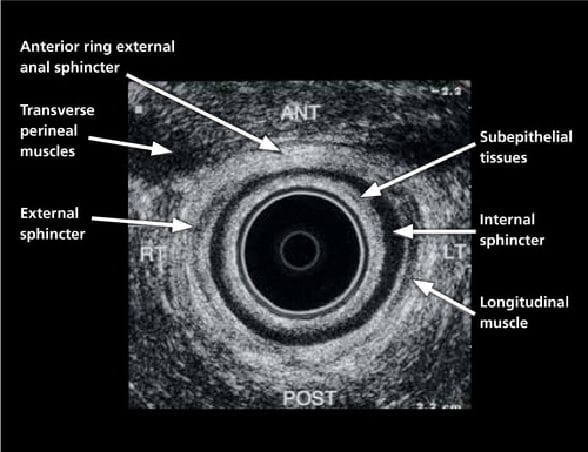
Anal physiology studies include endoanal ultrasound ,anal manometry; pudendal nerve terminal l motor latency and rectal balloon sensation. Endoanal ultrasound can determine the integrity of the sphincters :typically defects occur in the anterior half of the sphincter. St George Hospital has an excellent Anal Physiology Laboratory (tel: 85661000)
Obstetric-related Pudendal Neuropathies
The pudendal nerve innervates the EAS. Damage to the nerve can occur by stretching as it lies in the lateral vaginal wall after leaving the protective Alcock’s canal close to the ischial spines. It only needs 20% stretch over ?15 minutes to cause damage to the nerve.
Whilst 80% of these stretch injuries recover over ~10-11 months post partum the remainder do not recover and these manifest themselves as extreme rectal urgency. In some cases the warning to empty their bowel can be only a matter of seconds. In those cases the mother may be virtually confined to her home so that she is within metres of a toilet. It can transform a life :she can lose her career and isolate her from friends and family. It can destroy spousal relationships.
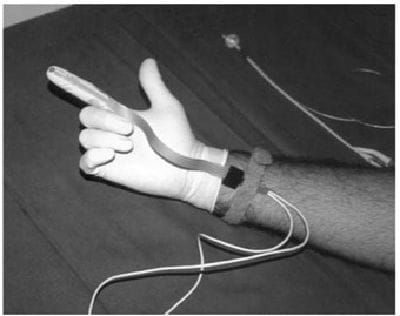
The proof of a pudendal neuropathy is helped by a pudendal nerve terminal motor latency test (PNTML) which measures the time taken in milliseconds for an electrical stimulus applied to the pudendal nerve near the ischial spine to reach a sensor adjacent to the anal sphincter.
Where recovery of the pudendal neuropathy does not occur then the insertion of a sacral nerve stimulator (SNS) can provide significant improvement or cure in 80% of cases.
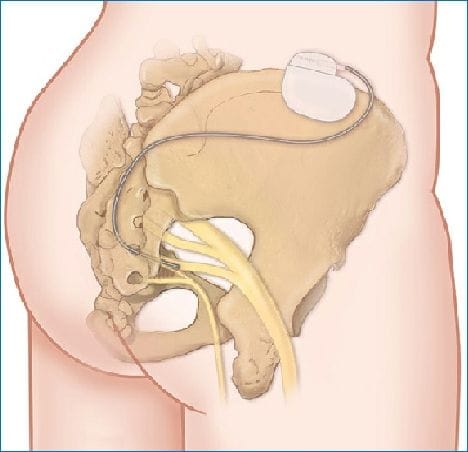
The sacral nerve stimulator is either a temporary (test phase) or a permanent implant into the skin of the buttock which delivers electrical impulses down a wire passed through the sacral foramen near S3 nerve root. The proportion of patients eligible for permanent implantation is approximately 50 per cent. The procedure is usually conducted under general anaesthetic and takes 2-2½ hours. It involves up to three incisions: one over the lower back to insert the lead into the selected sacral foramen, place it near the appropriate sacral nerve and anchor it; one in the lower abdomen or upper buttock to create a subcutaneous pocket for placement of the IPG; and a small flank incision to allow connection of the ends of the lead and extension, which the surgeon has tunnelled under the skin from the lead and IPG sites.
The battery lasts 5 years. The cost of these devices is considerable (~$20,000) but reimbursed at least in part through many private health insurers.
Further Reading:
- Alkharouf F, Joyce N, Ward D, Walsh F, Eogan M, Geary M. Trends in obstetric anal sphincter injury in spontaneous vaginal delivery versus operative vaginal delivery over a 10-year period: Lessons learned. Int J Gynaecol Obstet. 2023 May 26
- Abdool, Z.; Sultan, A.H.; Thakar, R. Ultrasound imaging of the anal sphincter complex: A review. Br. J. Radiol. 2012, 85, 865-875
- Steven Zhou, Lakshmi Akhila Nerusu, Nasir Hussain, Alaa Abd-Elsayed, Chapter 17 - Sacral neuromodulation, Editor (s): Alaa Abd-Elsayed, Neuromodulation Techniques for the Spine, Elsevier, 2024,
) Author:Dr Mike O'Connor
Author:Dr Mike O'Connor| Tags:Obstetrcis |








